
Why Your Migraines Keep Coming Back And What's Actually Causing Them
Waking up to a fourth migraine in seven days feels exhausting and confusing. You take medication, rest in a dark room, and follow every recommendation. Pain still returns within days. You probably keep asking the same question: why do migraines keep coming back when nothing seems to fix them long term?
Migraine recurrence rarely happens by chance. Most cases trace back to a hidden driver that pills cannot reach, usually rooted in the upper neck and cervical spine. Most doctors miss this connection completely.
Dr. Nicholas Belletto and the team at University Physical Medicine in Tallahassee see this pattern every week. Below, you will see what actually causes recurring migraines and why pain keeps returning.
Why Recurring Migraines Mean More Than Random Pain Episodes
Recurring migraines signal something specific. Most clinicians define chronic migraine as 15 or more headache days per month for 3 months or longer, with at least 8 of those days meeting full migraine criteria.
Episodes that keep returning rarely point to bad luck. According to the NIH National Institute of Neurological Disorders and Stroke, repeat migraine attacks usually involve the trigeminovascular system, where nerve and blood vessel signaling locks into an overactive loop.
Migraine episodes often unfold in stages: prodrome warning signs, optional aura symptoms, the headache attack itself, and a draining postdrome phase that can last up to a full day.
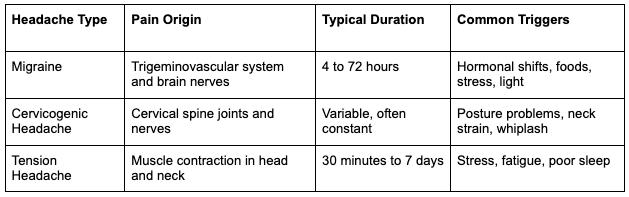
Knowing which type you have changes treatment direction. Patients with neck-driven episodes often benefit from reading how your neck might be triggering your headaches. Up next: four reasons migraines keep returning even when treatment seems to work.
Why Pills Cannot Stop Migraines From Coming Back Repeatedly
Pills mask symptoms but rarely fix the actual driver behind migraine attacks. So why do migraines keep coming back once medication wears off? Most cases trace to four factors that work in the background, often invisible to standard exams.
Untreated Structural Drivers in the Cervical Spine: Subtle misalignments in the upper neck irritate nerves that share signaling routes with migraine networks. Medication numbs the surface pain temporarily, yet the structural problem keeps firing signals through the trigeminovascular pathway. Until you fix the mechanical source through proper assessment, migraine attacks return on cycle no matter the prescription strength.
Sensitized Pain Pathways and Central Sensitization: Frequent migraine episodes train your nervous system to fire pain signals faster over time. Brain chemicals like CGRP keep flooding the system, lowering your threshold for the next attack. Each episode rewires your pain pathways, making future migraines easier to trigger and harder to stop with medication alone.
Medication Overuse Rebound Cycles: Taking acute migraine medication more than 10 days per month can paradoxically trigger more migraines, a condition called medication overuse headache. Your body adapts and starts producing rebound pain when the drug clears. Common culprits include triptans, combination painkillers, and daily ibuprofen used for headaches.
Unidentified Daily Lifestyle Triggers: Sleep position, jaw clenching, dehydration, and stress quietly stack up day after day. None of these alone causes a migraine, yet combined, they push your nervous system over the threshold repeatedly. Patients often blame random episodes when the real cause sits hidden inside their daily routine, quietly resetting recurrence with every overlooked habit.
Cervical spine drivers cause more recurring migraines than any other factor on the list. Why most doctors miss it comes next.
Why Your Cervical Spine Drives Most Recurring Migraine Pain
Most migraine patients never check their neck. Yet the upper cervical spine often controls the recurrence cycle through nerve pathways that medical workups overlook. Three structural issues drive most of these missed diagnoses.
How Upper Cervical Misalignment Activates Migraine Pathways
At the top of your spine, the atlas (C1) and axis (C2) sit just below the skull and connect directly to the brainstem. Nerves from both vertebrae merge with the trigeminocervical nucleus, the same neural hub that processes migraine pain. Even subtle misalignments fire signals your brain reads as a migraine attack rather than a neck problem.
Dr. Nicholas Belletto puts it directly: "Most migraine patients in our office show measurable upper cervical restrictions on their first exam. Once we restore proper motion, attack frequency drops significantly within weeks."
Standard MRIs rarely catch these mechanical patterns because imaging looks for tissue damage, not motion problems. Patients with this dysfunction often benefit from focused neck pain assessment to identify the exact restriction pattern driving recurrence.
Forward Head Posture And The Tech Neck Connection
Hours hunched over phones and laptops shift your head forward inch by inch. Each inch adds roughly 10 extra pounds of pressure on your neck and suboccipital muscles. Chronic compression irritates the same nerves tied to migraine attacks. Most patients call it tech neck without spotting the migraine link.
Watch for these warning signs:
Rounded shoulders that drift forward during work, scrolling, or driving cause persistent upper back strain that radiates into your neck.
Chin protrusion that pushes your face ahead of your shoulders creates direct pressure on cervical nerves during screen sessions.
Frequent suboccipital tension felt at the base of your skull by late afternoon signals nerve compression patients often overlook.
When Cervicogenic Headache Mimics True Migraine
Cervicogenic headache often disguises itself as migraine because pain spreads from neck to skull through shared nerve pathways. Diagnostic clues include pain starting at the base of the skull, limited neck range of motion, and pain consistently on one side of the head. Movement of your neck reproduces or worsens the headache, which rarely happens with true migraine.
Most neurologists miss this diagnosis because their workup centers on brain imaging and medication response, not cervical motion testing. Published research from NCBI shows manual orthopedic examination of the upper neck consistently spots cervicogenic patterns that imaging alone misses. Patients suspecting this overlap should look into chiropractic care for headaches and migraines for proper diagnostic clarity.
Why Daily Habits Cause Your Back To Back Migraine Attacks
Most patients hunt for one big trigger when migraines hit day after day. Reality runs deeper. Small daily habits compound silently and often cause back to back migraines, with most fixes starting inside your evening routine.
Sleep Position And Pillow Setup
Stomach sleeping forces your neck into 90 degrees of rotation for hours, compressing the same upper cervical nerves that drive migraine attacks repeatedly. Side sleeping with a firm pillow that fills the gap between your shoulder and ear keeps your spine neutral throughout the night. Wrong pillow height does the opposite: a pillow too thin or too thick creates the same compression as stomach sleeping all night.
Jaw Clenching And TMJ Overlap
Nighttime jaw clenching and bruxism keep the trigeminal nerve fired up for hours while you sleep. Pain from a tight jaw often shows up as a morning migraine on one side that pills cannot stop completely. Many Tallahassee patients reporting daily morning attacks grind their teeth without knowing it. Wearing a properly fitted night guard cuts TMJ migraine episodes for many of them within weeks.
Dehydration And Electrolyte Imbalance
Mild dehydration thickens your blood and reduces oxygen flow directly to the brain. Even small drops trigger a dehydration headache that can spiral into a full migraine flare up by evening. Common warning signs include:
Dark yellow or amber urine clearly signals your hydration runs below what your nervous system needs.
Afternoon brain fog and fatigue arriving between 2 and 4 pm often points to fluid loss, not sugar.
Recurring evening headaches that ease after drinking water confirm dehydration as the migraine trigger you missed.
Stress And Nervous System Overload
Chronic stress flips your sympathetic nervous system into overdrive and floods your body with cortisol day after day. Cortisol tightens your shoulders, tenses your jaw, and stiffens the deeper muscles around the upper cervical spine. Tight muscles then directly compress nerves that share signaling routes with migraine networks. Many patients feel attacks build the moment they finally relax on a Friday evening or Saturday morning, a classic letdown migraine pattern.
Why You Suddenly Get Migraines Every Day In Tallahassee FL
Patients walking into our office often ask: why am I suddenly getting migraines everyday after years of normal life? CDC data shows 1 in 6 American adults deal with migraine, but Tallahassee weather, pollen, and heat patterns push the number up locally. North Florida's environment stresses the trigeminal nerve, and your structural baseline decides whether you cope or break down.
Florida Humidity and Barometric Pressure Swings: Sudden drops in barometric pressure during Gulf summer storms make the trigeminal nerve fire more aggressively, a known barometric pressure migraine trigger. Tallahassee sees these pressure swings nearly daily from May through September, and patients with sensitive nervous systems feel each shift as a fresh migraine attack within hours of the front moving through.
Pollen Cycles and Sinus Pressure Migraines: Tallahassee's oak pollen season runs from January through April, with ragweed taking over by late summer, putting many residents under months of sinus pressure. Inflamed sinuses irritate branches of the trigeminal nerve and amplify migraine attacks. Patients who never had seasonal allergies before often suddenly start having daily migraines once their immune system shifts.
Florida Heat and Dehydration Cycles: North Florida heat indexes regularly cross 100°F from June through September, making Florida heat dehydration a daily concern for migraine patients. Even mild dehydration concentrates the blood enough to lower oxygen reaching the brain, a key humidity migraine trigger many patients miss. Drinking water alone falls short without electrolytes when temperatures climb that high outdoors.
Why Medication Patterns Quietly Reset Migraine Recurrence
Medication overuse headache, often shortened to MOH, develops when frequent acute migraine drugs alter the brain's pain signaling rather than calming it down. Roughly 1 to 2% of the global population lives with this condition, and most patients go undiagnosed for years.
Many cases of migraine recurrence trace directly back to MOH, a quietly progressive pattern that worsens the more pills you take. Triptan rebound and combination analgesic loops drive the largest share of cases worldwide.
MOH works through a straightforward mechanism. Frequent doses of acute medication train pain receptors to expect the drug, and when blood levels drop, those receptors fire harder than baseline.
Patients then take another pill, the cycle reinforces itself, and the underlying migraine driver continues firing untouched. Without intervention, the loop usually intensifies for months before patients even suspect their medication is the trigger.
Threshold rules count total dosing days across a typical month, not single use, and even occasional combination painkillers like Excedrin Migraine add up faster than most patients track. Watch how your daily count stacks against the chart below.
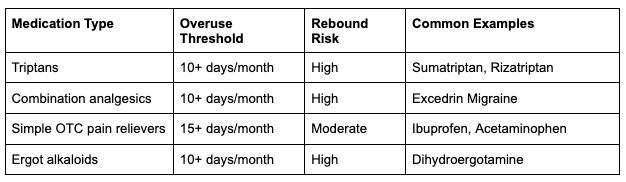
Suspect medication overuse headache when migraines hit more often, your prescription brings less relief than before, morning headaches arrive several days a week, and you reach for a pill before the previous one wears off. Patients stuck in this rebound headache cycle often find lasting relief through targeted structural care at our migraine relief center instead of climbing the prescription ladder further into chronic migraine territory.
Take Back Control From Recurring Migraines In Tallahassee
Dr. Nicholas Belletto and the team at University Physical Medicine in Tallahassee help patients break the recurring migraine cycle through targeted structural care, not stronger prescriptions. Anyone ready to look at options beyond medication can review the migraine relief options here and schedule a structural assessment.
FAQs
What causes migraines to come back over and over?
Recurring migraines usually point to untreated structural drivers in the cervical spine, sensitized pain pathways, daily lifestyle triggers, or medication overuse rather than truly random episodes.Can a chiropractor stop chronic migraine recurrence?
Chiropractic care addresses cervical spine issues, postural problems, and nerve compression, helping many patients significantly reduce migraine frequency once a skilled clinician identifies and treats the structural drivers.Why do migraines feel worse during humid Tallahassee weather?
Florida humidity creates rapid barometric pressure shifts that sensitize the trigeminal nerve, frequently triggering or worsening migraine episodes for many local residents throughout the summer storm season.Should someone with recurring migraines see a chiropractor or neurologist first?
Many patients dealing with recurring migraines start with a chiropractor for structural assessment, then add a neurologist if symptoms persist or warning signs continue to emerge.Are back to back migraines ever a sign of something dangerous?
Sudden severe migraine attacks arriving day after day, especially when paired with vision loss, weakness, fever, or speech problems, warrant emergency evaluation rather than waiting it out.